Two, Four, Six, Eight
This is how we intubate!
Yes, that’s a lame title, but I couldn’t think of a better. Sue me.
So you’ve got the gas, and it’s not good. It’s time to intubate the patient so they can be mechanically ventilated1. What does this look like? Well, you can be intubated emergently or not, depending how dire a shape the patient is in. Don’t get me wrong, if you need to be intubated there will be very little screwing around, but the doctor might be inclined to wait and get your or your family’s permission to hook you up to a machine—as opposed to, say, hospice. If they think the risk is too high and/or they can’t reach family that quickly, you’ll see a blurb in their notes later: “Procedure was conducted emergently; consent was implied.”2
(Intubation happens for a variety of reasons, which always boil down to “patient can’t breathe effectively” or “patient can’t be trusted to protect their own airway.” The OR intubates, and extubates, patients routinely, because an anesthetized patient can’t protect their airway. The anesthesiologist handles all that, and RT isn’t involved as a general rule. They have their own ventilators and everything down there, and we only hear about it when something goes a wee bit pear-shaped and we need to, for example, hook them up to one of our ventilators.)
For now, we’ll assume the intubation is emergent. Gather supplies! First, since it’s emergent, at most hospitals nursing will run and grab an RSI (Rapid Sequence Intubation) kit out of the med room. This box contains a couple of drugs needed to make it possible to intubate a patient humanely and safely. The exact ingredients will vary, but typically you’ll at least have some sedative and some paralytic3.
Respiratory needs a few more things than just that. For starters, a laryngoscope.
(Wikimedia commons)
Laryngoscopes became briefly famous during COVID; they look like tiny metal versions of the Grim Reaper’s scythe, and are used to hold the airway open and visualize the vocal cords so the person doing the intubation4 can stuff a tube in there. The illustration is of a scope with a curved “Macintosh” blade, but there’s also a straight “Miller” blade. They work slightly differently. Either way, they’ll have batteries in the handle and a little LED light at the tip of the blade.5
Obviously, you’ll need the tube itself as well. An endotracheal tube (ETT) for adult use can be in a variety of sizes, ranging from 6.0 to 8.5. That’s millimeters of inner diameter. The largest and smallest sizes are uncommonly seen; I’d estimate that more than half of all patients get 7.5 and most of the remainder wind up with 7 or 8. The determining factors are size of the patient and whether the doctor might want to do a bronchoscopy6 later. Small tubes create difficulties for a bronchoscope—or for an ordinary suction catheter, for that matter. More on that later.
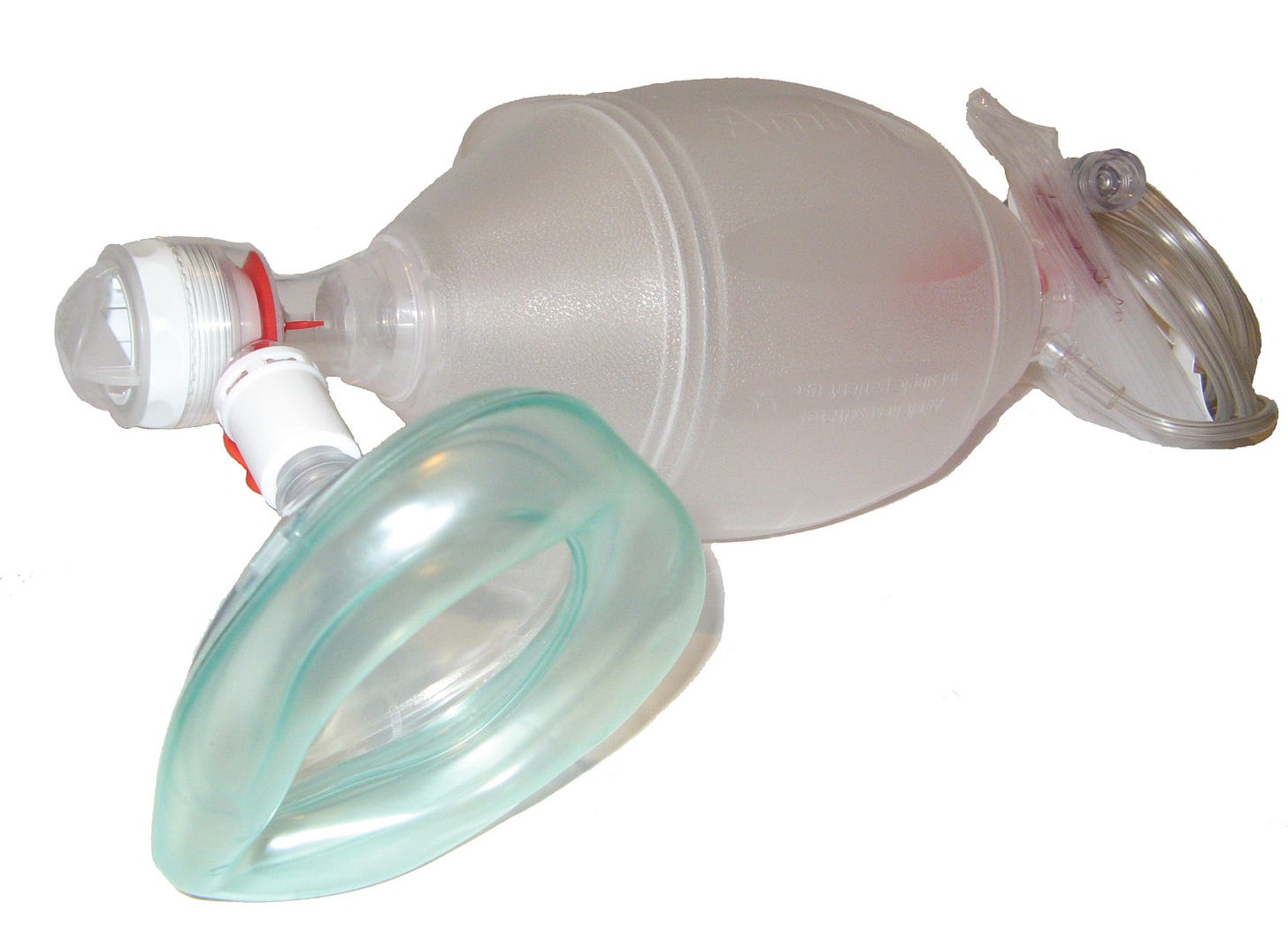
So, you’ve got the laryngoscope and the tube. But tubes are flexible plastic, and you’re trying to stuff it somewhere, so you’ll want a stylet, a semi-rigid rod of metal or plastic that fits inside the ETT to give it a backbone. You’ll also want a yankauer suction catheter hooked up and ready—think of the suction you get at the dentist, it’s similar—because you often need to suction secretions out of the mouth and throat so the tube can go through. And you’ll want a bag-valve mask, which … oh, hell, back to Wikimedia I go.
This one is courtesy of “Mike6271,” who uploaded it to Wikimedia back in 2008 but could conceivably still want credit. So, this is a bag-valve mask; it looks like it might be the familiar AMBU brand I always see7 in my hospital. The triangular greenish thing is the “mask” part, and goes over the patient’s nose and mouth. Once they’re intubated, the mask pops off and the tube it’s attached to fits neatly around the end of the ETT. The coiled-up tubing at the end connects to an oxygen tank or wall outlet, cranked up as high as it will go (“flush” is the term we use for that). The tubing is wrapped around a crinkly bag, which inflates once gas is flowing through8. The football-shaped thing in the middle is what you squeeze to manually force in a breath.
Moving on! You’ve got a tube, a stylet, suction, and a bag, but you’re still not done. You also need a syringe—not a needle, the syringe a needle screws onto, typically 10 or 12 cc’s capacity. Ideally, you should also have a disposable capnometer to confirm successful placement, and some doodad to hold the ETT in place once they’re intubated; we use Hollister-brand holders which stick to your cheeks with adhesive pads, but the old-fashioned way is to wrap it up with tape, and ole grandpappy RTs will still know formidable levels of tape-fu such that they can rig up a complex harness out of tape in a couple of minutes.
Oh, and you’ll also want somebody to get a ventilator while all this is going on, unless you plan to sit there manually bagging the patient forever. Which, I mean, it’s an option. You could. Hand might get tired after half an hour or so. Your fault for signing up at a facility too cheap to get a fleet of ventilators.
Now, that’s a lot of stuff to assemble, isn’t it? Which is why smart RTs will at the very least have it all assembled beforehand so you can just grab a bag. Or, if your facility has moved on since the 1990s, you might have a Glidescope cart. Just going to link to it this time. Glidescope is the “easy” button. There’s a tiny camera on the end of a disposable hook-shaped apparatus, such that you don’t have to actually be eye-level with the patient’s airway. You can just look at the screen to guide tube placement, which is far easier and more comfortable. Almost nobody uses the old manual laryngoscopes anymore. My hospital has one ER doctor who’s too cool for the Glidescope, because he’s proud of his old-school skills or something.
Anyway, we keep the Glidescope cart9 stocked with all the accessories I just named, including a selection of old-fashioned laryngoscopes in case the Glidescope stops working, which I’ve never seen happen yet. The “crash cart” used in codes will also have a variety of airway management devices in one drawer (the rest of the drawers are full of Nursing Crap like drugs and saline).
For explanation purposes I’ll pretend we’re at an underfunded facility which doesn’t have a Glidescope. Suction is set up, bag is running, tube is present with stylet and syringe, consent is obtained or implied, doctor is present, patient is drugged or so out of it he doesn’t need drugs, okay, go. The doctor-or-other-intubating-person stands at the head of the bed, behind the patient’s head, and the RT passes them stuff.
The laryngoscope is held in your non-dominant hand with the blade sticking out the bottom of your fist, facing towards the patient. You put the blade10 in the patient’s mouth to scoop the limp tongue out of the way, tug upwards at an angle to get things open, and visualize the vocal cords, gateway to the trachea. This gateway has a gatekeeper known as the epiglottis, a little flap of cartilage that exists to keep food and water from going down into the lungs. If you’re looking down with a laryngoscope, the “hinge” of the epiglottis is at the top (in medical jargon, it’s anterior, in the direction of the face and the front of the body).
If you’re using a Macintosh or “Mac” blade, the end of it will stick right into a notch called the vallecula, right above the hinge of the epiglottis, and the tugging motion described earlier will indirectly force the glottis to open by applying pressure to the vallecula. If instead you have a straight “Miller” blade, the blade will simply ram its way through and force the epiglottis up directly. I’m sorry if this is hard to visualize without pictures, but I’m proceeding under the assumption that you are not planning to do this yourself based on stuff you read in some weirdo’s Substack11.
If you can see the vocal cords, it’s a straight shot. You (the doctor or whoever) ask for the scope, without taking your eyes off the vocal cords. The RT puts it in your hand, and you shove it through the vocal cords. Once it’s in, the RT uses the syringe to inflate the cuff at the bottom of the ETT (referenced in my post on trachs), and pulls out the stylet. Then the RT takes the mask part off the Ambu bag and puts the disposable capnometer in-line. There are different models of disposable capnometer, but they’re all cheap clear plastic and have a part that fits your bag and a part that fits the end of the ETT. You squeeze oxygen in, and something inside the capnometer hopefully changes color (in reaction to exhaled CO2). If it doesn’t, you probably stuck the tube in the stomach and should stop bagging, because air in the stomach tends to induce vomiting and vomiting now would be very, very bad. Take the tube out and try again.
Assuming you got the ETT in the trachea, you listen to both lungs with your stethoscope12. This confirms, again, that you’ve got the tube in the right place, and also that you didn’t stick it down too far such that you’re only ventilating one lung—the natural curvature of the airway tends to encourage the tube to go to the right lung if you’re too deep. You may need to deflate the cuff, pull it back a couple of centimeters, re-inflate, and check again. The doc will be ordering a stat chest X-ray to confirm in any case.
If all of that checks out, you look at the monitor and say, “tube is a 7.5 at 23 at the teeth13, time of intubation is 1817 … ugh, why do patients always have to crash right at shift change?” Then somebody squeezes the bag while somebody else secures the tube with your disposable device or convoluted tape harness. Then you hook them up to the vent with appropriate settings, throw away various forms of medical trash14, and go chart what you did.
All that should have taken place within, oh, five minutes or less. This is just the beginning.
If the gas is only middling-bad, you can try BIPAP, or non-invasive ventilation, first. BIPAP uses a mask strapped tightly to your face. Sometimes it works incredibly well, sometimes it fails pathetically. But it’ll be the subject of a full post at some later date, I’m sure. For now, full-on invasive mechanical ventilation!
People who need intubation are very commonly unable to think or communicate their wishes clearly. This may be the reason for intubation—patient is obtunded and unable to protect their own airway—or a mere side effect of severely acidic blood (acidosis).
A note on paralytics such as rocuronium or succinylcholine: they paralyze ALL the muscles over which you have any voluntary control, including your diaphragm, but do not sedate you at all. Being paralyzed but not sedated is some body-horror material. If you paralyze, you must sedate in addition to manually or mechanically ventilating the patient. There was a middling-famous case a while back where an overworked nurse administered vecuronium (paralytic) instead of versed (benzodiazepine sedative related to valium). As you might imagine, the patient died horribly.
Typically a doctor or nurse practitioner, but RTs are licensed to intubate, as are paramedics if it happens inside their ambulance. It might not be the custom for RTs at a given facility; I have been an RT for almost five years and never intubated a live human. I’m a little salty about it, honestly, but there’s seldom a need for it.
Old-fashioned laryngoscopes like these have expiration dates—I guess the prepackaged batteries can only be guaranteed to hold a charge so long? When they expire and we’re going to throw them out, I bring them home. They make fun reading lights and flashlights in addition to being very handy for, say, spotting something under the fridge. If it involves peering into a dark narrow space, a laryngoscope is good for it.
Stuffing a fiber-optic probe down into the lungs to clean them out and/or diagnose a problem. Again, a whole post unto itself.
As in, “dammit, he’s fading, get me an AMBU.”
Unless you are on a medical TV drama, in which case the bag will be limp and empty while serious-looking actors in paramedic costumes squeeze it and snap at each other about how there’s no TIME, the patient needs [procedure] NOW. The RTs in the audience will be laughing, because that patient is probably not oxygenating very well. Now you can laugh too!
Glidescope is a registered trademark of somebody or other but I’m damned if I’m going to bother with the little R in a circle. Sorry, capitalization is all you get, uh … Verathon corporation, or whoever. BIPAP, referenced in the first footnote, is technically also a trademark of Respironics (I think) but has long since been genericized to mean any non-invasive ventilation device, the same way we say “Kleenex” for any kind of disposable tissue.
In the unlikely event this is not obvious to you, it is called a blade because it is blade-shaped. It is not sharp. That would be terrible.
Don’t. Or, if this warning comes too late and you are already mid-intubation, please stop, get a physician, then get a lawyer.
I didn’t list the stethoscope in parts needed, but you should always have your stethoscope handy. Unless you’re the doc/NP, who forgets half the time and asks to borrow yours so they can listen.
The ETT is about a foot long, its sides marked with centimeter markings. We refer to patients as being “[tube size] at [cm marker closest to] at [lip or teeth/gums, I prefer the latter since lips are floppy].” This is important since a poorly secured tube can slide up or down, or be forced gradually out by a feisty or poorly sedated patient. So you document where the tube is, every check. PROTIP: almost everybody is a 7.5 @ 23 or thereabouts. Short people might be a 20 or 21, tall people might be 24 or 25, but it all clusters around 7.5 @ 23.
Or maybe don’t, if it’s the ER. They’ll just leave trash lying around and hope/assume that Environmental Services will get it in a couple of hours after RT wheels the patient up to the ICU to be somebody else’s problem. ER turnover is way too high to be bothering with all that.