My Job Sucks
Can I say just one word? Sputum.
Content warning: yucky stuff.
I said in an earlier post that Respiratory exists as a separate discipline from nursing because most nurses are scared of snot. I was joking—partly. A large share of nurses really do seem to be unusually scared of sputum1, which is fascinating to me because they’re not uncomfortable around any other body fluid or, ah, substance. Nurses deal with all of them—including sputum, because airway management is often a shared responsibility between our disciplines—and they do some, to me, truly disgusting things, up to and including disimpaction2. They regularly and more or less dispassionately wipe butts, and to the extent the task irritates them a lot of the irritation seems driven by the addition to their workload. But sputum? Ewwwwww. I’ve asked my veteran RN mother to explain it. She can’t, but she agrees: sputum is simply too gross. Possibly because it’s the one fluid whose management can regularly be left to us, so they’re not used to it?
Whatever the case may be, respiratory deals with it. A lot. Particularly if you’re working the ICU that day, your job as an RT is going to entail a lot of converting “mucus” to “sputum” by mechanical means, for those who can’t do it themselves. One of my RT School professors referred to the gurgling. slurping noise of snot through tubing as “the sound of money.” So I thought we might spend a post going over the wonderful world of suction.
For starters, where does suction come from? Well, in an inpatient setting, you often encounter fluids that need to be removed from the body by suction, either occasionally or continuously3, so as a rule every hospital room comes equipped with suction standard. There are color-coded outlets at the head of the bed—green for oxygen, yellow for medical air, white for vacuum—and all you need to do is plug in the appropriate regulator or adapter, then whatever device you need to blow air or oxygen or suck things away45. The white vacuum one connects to a regulator, which connects to a short length of plastic tubing, which connects to a canister to hold whatever you’re sucking—I assume so you needn’t worry about it gumming up the regulator—which connects to a much longer bit of tubing, which connects somehow to whatever goes in the business end.
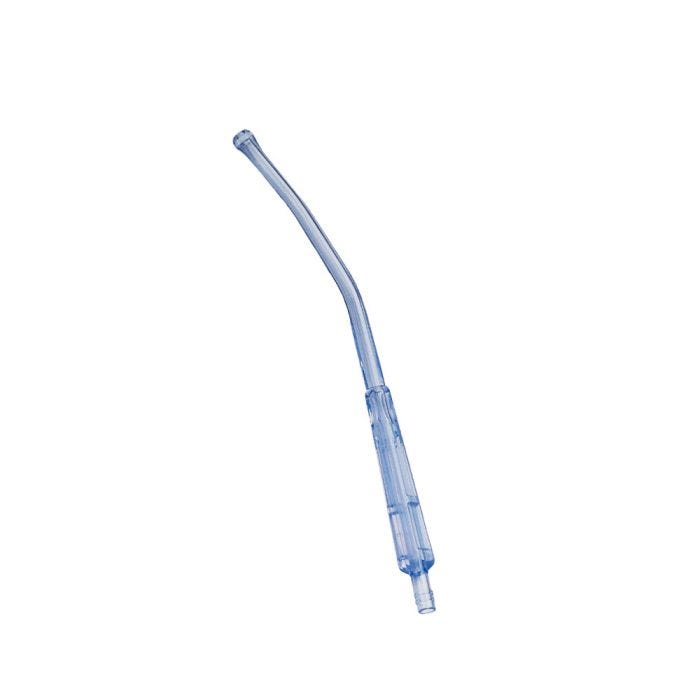
Sometimes the last part of the chain is a humble Yankauer6 suction tool, a disposable plastic wand the patient can use themselves.
(From “bettersupport.com.au,” apparently, but there are like a billion medical supply sites out there with extremely similar images.)
The Yankauer is made of hard plastic, has a rounded bulbous tip so it’s hard to accidentally cut the patient with it, and curves forward to follow the normal curvature of your tongue and throat. If need be, I can stick this thing in a severely confused patient’s mouth and hoover up gunk from the base of their tongue—if you stay low, the risk of triggering the gag reflex is less than you’d expect—but I also like to grab one of these for patients who can almost, but not quite, cough stuff up7.
That latter approach takes time, but that’s part of the appeal of it, for me. I have to hang out with the patient while they’re doing a neb treatment anyway; I can either finish typing up my simple notes and then stare at them like a weirdo, or I can say, “hold on, I’ve got something that might help with that,” then haul in a canister, a regulator, two tubes and a good ol’ Yank-yank8.
All the while the neb is running they watch me snap the lid on the canister, plug in the tubes and the adapter, and verify that the system works. This is pretty easy once you’re used to it but it looks like an intimidatingly complex task to a layman, which shapes their expectations for the future. They can think, “wow, this guy is going to a lot of effort, I’m at a good hospital being taken care of” or “wow, this guy is going to a lot of effort, I’d better put equal effort into getting better so as not to waste that” or “wow, this guy is going to a lot of effort, this an advanced and powerful system and I am going to beat this personal problem with the help of my support staff.” All three are very good thoughts for a patient to have, and will make it easier for me to treat them and for them to recover.
Whatever they’re thinking, once I’m done they have a tool that gives them something to do other than sit around moping and watching bad TV, which gives them a sense of agency. With practice they get quite accustomed to shoving this thing way back there, coughing, and hopefully catching the loogie before it slides back down to its annoying little home just above the vocal cords.
If the patient is weak and possibly confused, I can do it myself, but a Yankauer isn’t always enough. Sometimes it’s too far down, or the patient is too feisty and won’t open their mouth, etc. Then you get into nasotracheal suctioning, which involves a disposable flexible catheter and a packet of lube. The catheter comes in a small pack with a pair of sterile gloves9. You take out the gloves in their paper wrapper, squirt a packet of medical lube in the bottom of the (still sterile, unless you touch it) pack, and … yeah. In through whichever nostril is more conventient—sometimes there’s an O2 cannula or nasogastric feeding tube in the way—and down, down, down. You have a “clean” hand and a “dirty” hand. The former should only handle the flexible catheter itself; the latter is holding the suction tubing where it attaches to the catheter, and manipulates the thumb switch. Once you’re far enough down—which can involve more guesswork than I like, frankly—you hit the thumb switch and start drawing the catheter back out. Sluuuuuuuuuuuurp. The patient is usually struggling mightily through all this and may need to be held down, because it isn’t fun at all.
Having described all that: NT suctioning is very much a double-edged sword, and I don’t like it or do it for basically any reason short of a direct order from a doctor. I mean, you need a doctor’s order to do it at all10, but it’s usually not worth it, because discomfort aside, no amount of lube is going to make NT suctioning non-traumatic, and if you start a bleed halfway up their nose where you can’t reach to stanch it, it’s all going to trickle down, usually backwards. Now the patient has bloody unmanageable secretions. Great job, Doctor Jackass. Besides, if secretions accumulate once, they’re going to accumulate again, unless the patient gets better mentally or physically, and they usually don’t once they get that bad11. You’re bailing out a boat with a hole in the bottom. Are you just going to keep bailing it forever? What’s your endgame here? This can be somewhat mitigated with a “nasal trumpet” inserted into one nare and left there, but … nah. Let’s just not go there.
Everything gets much simpler once the patient is trached or intubated. A tracheostomy establishes a mercifully short and dedicated passage to the lungs; not only is it easier for the patient to cough gunk up and out, the same catheters used for NT suction can be employed to snatch anything they can’t expel from their lungs. Quick and easy, no risk of damage to the upper airway which you’re bypassing entirely.
Easier still: patient is on the vent. Not going to dig up a second picture, but the ventilator circuit approaches the patient’s ET tube from the side, and makes a right-angle turn to get in through an in-line suction catheter setup. The catheter itself is left dangling from the end of the setup, inside a flexible sleeve. When you need to suction a ventilated patient, you hit the 100% O2 button on the vent (since suction tends to promote hypoxia), which depending on vent age and model may also pre-silence the alarms (the vent can tell when the airway is occluded since pressures go up, but it doesn’t know what’s causing it). Then you grab the dangling catheter and shove it down the ET tube, quickly but carefully. If the patient has a cough or gag—not all do, for reasons of neurological injury, deep sedation, or both, and if they don’t you go by depth—you hit the button to activate suction once they react, then draw back, same as with the disposables.12
You want to draw back slowly, and maintain suction the whole time. RT school may teach you to rapidly flick the switch so it makes a sputtering noise, but that’s dumb. You’re just going to drop the goods that way. And for heaven’s sake do it at a reasonable, slow speed, unless the patient is in absolutely terrible shape. Nurses tend to zip it back out in less than a second, and barely get anything. Every time you suction, you’re risking damage from the catheter bonking into the carina where the trachea bifurcates to go to the lungs. The airway isn’t built to hold up under much bonking, so if you’re going to suction, make it count!
Sometimes, routine suction isn’t enough. Ventilator circuits are, or should be, heated and humidified13 but that can only do so much and often the lungs get hard, dry, occluding mucus plugs that raise pressure and impede performance. For this, we have lavage14. The in-line catheter has a dedicated port where you can attach a “flush” syringe full of saline. Silence vent. Put flush in line. Run catheter all the way down, then squirt and pull back. This is scary to a lot of nurses—you’re putting liquid in their lungs—and I don’t do it routinely, but when it works and you actually hear the distinct rattle of a plug or five going through your tubing—mmmm!
That’s the sound of money, baby.
Secretions from the lungs, once they have left the lungs. Before that, they’re “mucus” or just “secretions.” Kind of like “lava” and “magma.”
If you don’t know what that is, sometimes the only answer to sufficiently severe constipation involves a nurse with a very long glove.
Among other examples, chest tubes for fluid around the lungs, drains for wounds, and more prosaically, various apparatus to get rid of urine before it makes a mess of the sheets. It’s possible you’ve seen ads for the “PureWick at home” system for incontinent seniors, featuring a smiling old lady playing cards with her daughter. It plays on the hospital TVs all the time. I always wonder if PureWick at home is quieter than PureWick at the hospital, or if the daughter is just discreetly ignoring the loud rattling gurgle as she calls out “rummy!”
You have to plug a flow regulator into the wall to get oxygen to connect to a nasal cannula or mask. The regulator isn’t built into the wall because ventilators and other devices just plug into the same outlets directly. Shove a hose in. As a safety feature, medical air and oxygen use different socket arrangements such that you absolutely cannot plug a hose or regulator intended for one into a wall socket which produces the other. I don’t think yellow-green colorblindness is a serious issue in healthcare but it could be an issue in a dark room, or a hurry, or both.
Also, incidentally, there are about a billion power outlets. The red ones are backed up by the hospital’s generator, for devices that must not be allowed to fail. Such as ventilators!
Routinely pronounced “yanker” here in the Deep South, except by me. I resolutely pronounce it “YAWN-cow-er” because I feel ignorant saying yanker. It’s not spelled that way, dammit. Almost everyone knows what I mean from context, but if they don’t, I will absolutely die on this hill. It’s a YAWN-cow-er, or possibly YAN-cow-er but the former feels more correct from what I know of German/ic pronunciation. Fight me.
This standard model of Yankauer has a thumb switch you can’t see in the picture, consisting of a hole on the back near the top of the “handle” part. Unless you cover it, it will suck out of that hole, not the tip. If I’m giving one to the patient, I wrap tape around it so they don’t have to bother with that.
There’s also a second model of Yankauer with an opaque blue handle, a sliding thumb switch, and a flexible plastic sleeve you can use to cover it up and set it down without exposing this thing that goes in your mouth to hospital bed (or, if you drop it, hospital floor) germs. Much nicer and more user-friendly, but I don’t like using it myself because it lacks the bulbous tip and confused patients tend to struggle with surprising vigor when you violate the sanctity of their oropharyngeal cavity.
YAWNK-YAWNK!
The gloves come prefolded in a specific way with the cuffs rolled up, so with practice you can put them on quickly without compromising the sterility of their external surfaces. Some RTs don’t bother since NT suctioning is a clean but not sterile procedure. I always stop and glove up, for several reasons. First, because it’s fun. Second, because every little bit of sanitation helps. Third, because it wordlessly communicates professionalism and reassures the patient, at very little cost in time.
I hope all this expectation-management doesn’t come across as cynical or manipulative. I suppose it is the latter, in a way, but it’s a subset or variant of what Discworld readers may recognize as Weatherwaxian Headology. Perceptions shape expectations and expectations shape reality. I’m aiming for reassurance, not insincerity. Hospitals are scary.
Nurses tend to ignore that requirement, for whatever reason. They can if they want. I’m protecting my license, thank you.
My experienced coworker—the one I adopted as my “sensei” when I started at my second hospital with a year under my belt—refers to that horrible loud gurgle you can hear from the door as “death rattle.” “You can’t fix death rattle,” he says, and in my experience he is correct. Chronically unmanaged secretions are a harbinger of death.
EDIT: Reviewing this, the description might be confusing to non-RTs who’ve never seen this setup, but honestly the pictures I’ve found with a cursory googling don’t look helpful to the layman either. Basically the catheter is set up so it’s in a straight line with the end of the ET tube, and the plastic sleeve around it bunches up as you shove the catheter in. The whole thing is set up so you can suction at will without having to break the circuit and introduce outside germs to the system (or the patient’s germs to the outside world). Let me know if any of this is still unclear. Oh, or look at these things.
My first hospital used HMEs, heat-and-moisture-exchangers, because it was rural and poor, but this is not anywhere near as good as real heated humidification, particularly for longer-term use. An HME is like putting a sock over the patient’s mouth to trap the humidity of their own breath inside. It’s, strictly speaking, better than nothing at all, but ugh.
Unlike the poor Yankauer, everyone pronounces this in the correct Frenchified manner, luh-VAHJJ, because we’re fancy like that. It just means “washing,” of course.